|
8/26/2023 0 Comments Dead space vs shunt usmle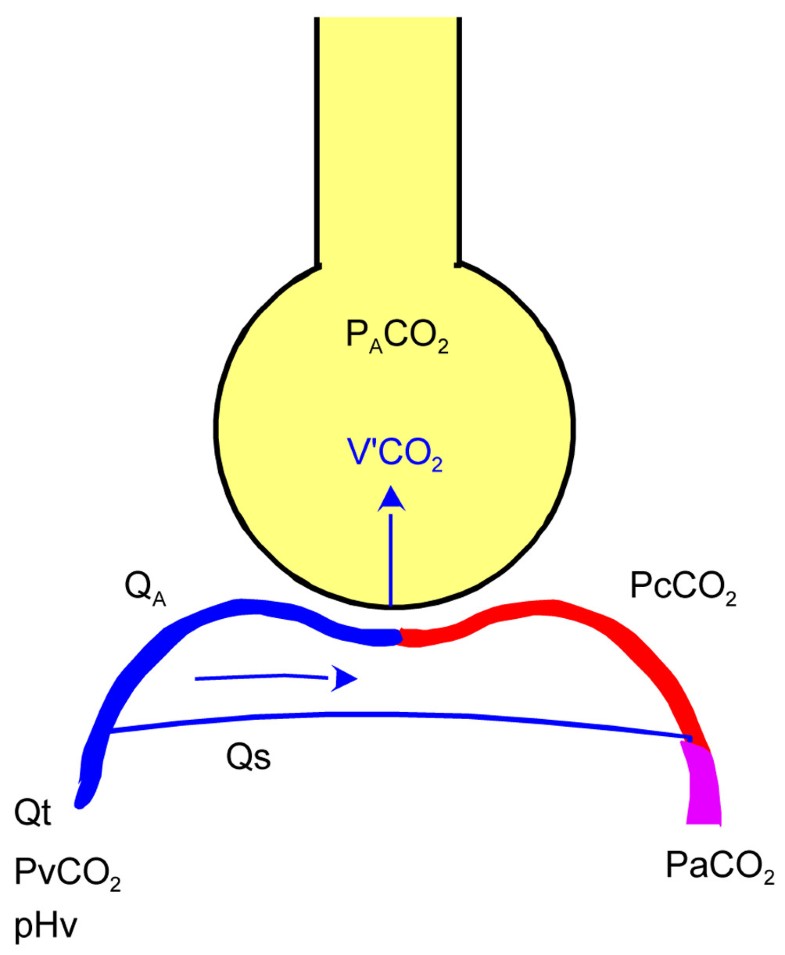
Use of accessory respiratory muscles due to diaphragmatic dysfunction.Asynchronous movement of the chest and abdomen during respiration.Barrel ches t : This deformity is most commonly seen in individuals with emphysema.Prolonged expiratory phase, end-expiratory wheezing, crackles, muffled breath sounds, and/or coarse rhonchi on auscultation.More commonly seen in patients with emphysema.This style of breathing increases airway pressure and prevents bronchial collapse during the last phase of expiration.The patient breathes in through the nose and breathes out slowly through pursed lips.Chronic cough with expectoration (expectoration typically occurs in the morning).Symptoms are minimal or nonspecific until the disease reaches an advanced stage. Imbalance of oxidants and anti-oxidants and an overabundance of free radicals → chronic inflammation and inactivation of anti- elastase → breakdown of elastic tissue.Pulmonary shunt and ↓ blood volume in pulmonary capillaries → ↑ number of alveoli that are ventilated but not perfused ( ↑ dead space) → ↓ DL CO and ↑ V/Q → hypoxemia and hypercapnia.Enlargement of airspaces → ↓ elastic recoil and ↑ compliance of the lung → ↓ tethering of small airways → expiratory airway collapse and obstruction → air trapping and hyperinflation → ↓ ventilation (due to air-trapping ) and ↑ dead space → ↓ DL CO and ↑ ventilation-perfusion mismatch (V/Q) → hypoxemia and hypercapnia.Nicotine use (or other noxious stimuli) inactivates protease inhibitors (especially α 1-antitrypsin ) → imbalance of protease and antiprotease → ↑ elastase activity → loss of elastic tissue and lung parenchyma (via destruction of the alveolar walls), which causes:.Bronchopulmonary inflammation → ↑ proteases.Smooth muscle hyperplasia of the small airways and pulmonary vasculature (mainly due to hypoxic vasoconstriction ) → pulmonary hypertension → cor pulmonale.Reid index > 0.5 is characteristic of chronic bronchitis.Reid index is the ratio of the thickness of the submucosal mucus-secreting glands to the thickness between the epithelium and cartilage in the bronchial tree.Promotion of goblet cell proliferation and hypertrophy, mucus hypersecretion, and impaired ciliary function → chronic productive cough.Overproduction of growth factor → peribronchiolar fibrosis → narrowing of airway → obliteration → emphysema (airflow limitation).CD4+ T lymphocytes and eosinophils mediate inflammation in individuals with bronchial asthma.CD8+ T lymphocytes mediate inflammation in individuals with COPD.Increased number of neutrophils, macrophages, and CD8+ T lymphocytes → release of cytokines → amplification of inflammation and induction of structural changes of lung parenchyma (e.g., via stimulation of growth factor release).It results from significant exposure to noxious stimuli, increased oxidative stress (most commonly due to cigarette smoke) as well as by increased release of reactive oxygen species by inflammatory cells. The most significant complication is acute exacerbation of COPD.ĬOPD is characterized by chronic airway inflammation and tissue destruction. COPD can cause complications such as pulmonary hypertension or respiratory failure. Individuals with advanced disease may benefit from oxygen supplementation and/or noninvasive ventilation. Treatment options mainly consist of short-acting and long-acting bronchodilators and inhaled corticosteroids. Imaging studies are helpful in assessing disease severity and the extent of possible complications. Diagnosis is primarily based on clinical presentation and pulmonary function tests ( PFTs), which typically show a decreased ratio of forced expiratory volume ( FEV) to forced vital capacity ( FVC). Clinical features include dyspnea and productive cough and, in later stages, tachypnea, tachycardia, and cyanosis. These changes cause a loss of diffusion area, which can lead to inadequate oxygen absorption ( hypoxemia) and CO 2 release ( hypercapnia). COPD begins with chronic airway inflammation, which usually progresses to emphysema, a condition that is characterized by irreversible bronchial narrowing and alveolar hyperinflation. Some individuals are genetically predisposed to COPD, particularly those with α 1-antitrypsin deficiency ( AATD). It is predominantly caused by inhaled toxins (e.g., tobacco smoke or air pollution). Chronic obstructive pulmonary disease (COPD) is characterized by chronic respiratory symptoms resulting from airflow obstruction and alveolar gas exchange abnormalities.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
